Biliopancreatic Diversion With Duodenal Switch (Single Anastomosis)
The traditional duodenal switch with biliopancreatic diversion (DS/BPD) was first introduced in 1986. It is a complex bariatric surgery that has not been widely implemented despite its excellent results and long term weight reduction success. Due to this a simple version of the duodenal switch was introduced over 5 years ago, the loop DS or the SADI. 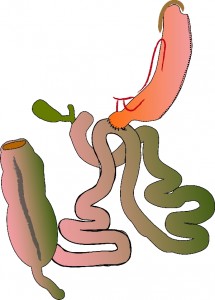 The SADI (single anastomosis duodenoileostomy) is a type of duodenal switch bariatric surgery that involves a loop anastomosis rather than traditional roux reconstruction. There are two parts to the surgery. First, a sleeve gastrectomy is made to reduce the size of the stomach. Second, the duodenum is divided just beyond the pylorus. The lower part of the intestine, the ileum is anastomosed to the duodenum at a length of 250cm from the terminal ileum. The bile and pancreatic enzymes will empty their normal route(afferent limb). Digestion of protein and fat now take place in a common channel. SADI is a new form of Duodenal Switch which has been around for just over 5 years. The fundamental differences between conventional DS and SADI are:
The SADI (single anastomosis duodenoileostomy) is a type of duodenal switch bariatric surgery that involves a loop anastomosis rather than traditional roux reconstruction. There are two parts to the surgery. First, a sleeve gastrectomy is made to reduce the size of the stomach. Second, the duodenum is divided just beyond the pylorus. The lower part of the intestine, the ileum is anastomosed to the duodenum at a length of 250cm from the terminal ileum. The bile and pancreatic enzymes will empty their normal route(afferent limb). Digestion of protein and fat now take place in a common channel. SADI is a new form of Duodenal Switch which has been around for just over 5 years. The fundamental differences between conventional DS and SADI are:
- There is only one (1) with the anastomosis SADI compared to two (2) for the DS
- With the SADI, there is a longest common loop through which nutrients pass, which causes a decrease in stool frequency, fewer side effects and less deficiencies in vitamins and minerals for the SADI compared to DS.
Advantages
- On average, the surgery lasts less than two hours and patients get their discharge from hospital after 1-2 days of the operation.
- Patients can resume the work 2 to 4 weeks after surgery.
- Greater weight loss than the Sleeve and the roux.
- Surgery effective for lowering cholesterol and triglycerides.
Disadvantages
- May result in weight loss slightly less than the DS.
- The long-term outcomes are still evolving.
Risks
- Intestinal obstruction: 2-4% of reported cases.
- Require repair due to malnutrition: 1-3% of reported cases.
- Leaks: <1% of reported cases.
- Bleeding: <1% of reported cases.
